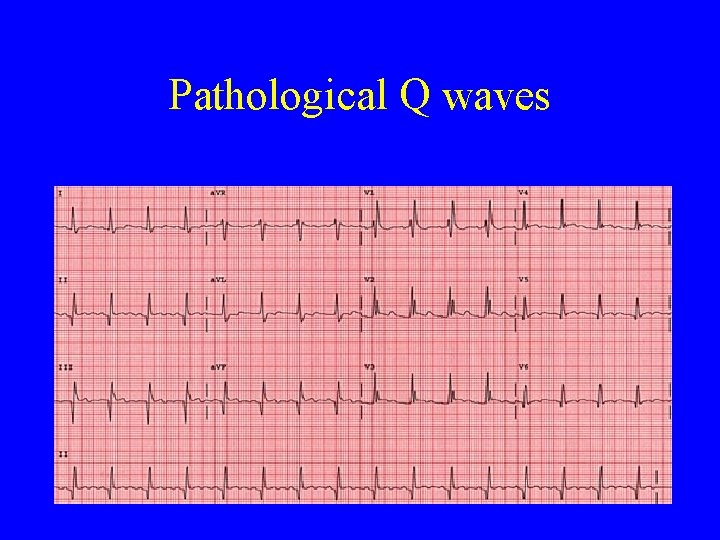
Whether some high risk subgroups will benefit from any of these strategies remain a subject of debate. The latter goal has been more elusive, since large randomized trials have failed to show benefits from preoperative coronary revascularization or perioperative beta blockade, or by extension the preoperative testing that might refine risk stratification. The former goal has been achieved, as numerous studies have validated the Index, even if some have suggested ways to improve it in certain types of patients. Width: 0.03s Depth: of QRS amplitude Needs to be present in at least 2 neighboring leads. Q waves in leads other than the above can be considered pathological, particularly if they are: >2mV / small squares deep or >25 of associated R wave and/ or >0. Width: 0.03s Depth: of QRS amplitude Needs to be present in at least 2 neighboring leads. We had hoped that the Index would not only estimate risk but also help target certain subgroups of patients for specific beneficial interventions. T Waves QT intervals Patterns > Interpreter Pathological q Waves. Furthermore, the original index changed practice, so that previously important factors (recent MI, severe aortic stenosis) were rarely represented in the more recent cohort of patients. As a result, evidence of coronary disease and heart failure replaced prior reliance on the arrhythmias (both atrial and ventricular) that had been very important in the original index. The revision was important because of major changes in the diagnosis of cardiac disease during the intervening years – especially the widespread use of echocardiography and less use of Holter monitoring. The Revised Cardiac Risk Index was published 22 years after the original index became the first multifactorial approach to assessing the cardiac risk of non-cardiac surgery and one of the first such approaches for any common clinical problem. Septal Q-waves are small, nonpathological Q-waves <0.03 s and. Lee Goldman on original Goldman Cardiac Risk Index for MDCalc: A Q-wave may also be normal in aVL if the frontal QRS axis is between 60o and 90o. with serum NT-proBNP or BNP) and determine appropriate cardiac monitoring post-op (EKG, troponins).Īlternative perioperative cardiac risk scores like the Myocardial Infarction and Cardiac Arrest (MICA) Score and the American College of Surgeons (ACS) National Surgical Quality Improvement Program (NSQIP) Score have been validated only retrospectively and therefore underestimate the risk of myocardial ischemia ( Duceppe 2017, Rodseth 2014, Devereaux 2011) compared with the RCRI, which has been validated by multiple studies over the past 15 years including a very large 2010 systematic review (24 studies and 792,740 patients) which found moderate discrimination in predicting major perioperative cardiac complications ( Ford 2010).ĭr. In patients with elevated risk (RCRI ≥1, age ≥65, or age 45-64 with significant cardiovascular disease), helps direct further preoperative risk stratification (e.g. Accurately risk-stratifies patients and helps patients understand individualized risk prior to undergoing surgery, which can be helpful in discussions of informed consent.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
